I Have Gallstones! Should I Get Operated?
December 26, 2019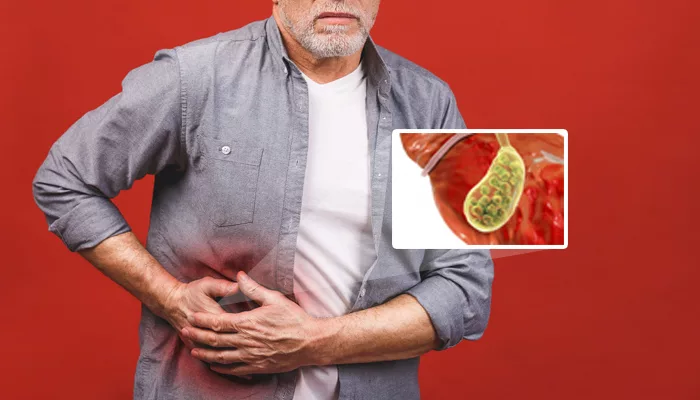
This is how you would normally describe your symptoms to your doctor. “I have gas problems. Sometimes, not often, maybe after eating out, maybe after that chicken tikka we had last night? That was a little too much. Now I feel bloated.” It is usually ‘OK’ in a few hours’ time. Daily work life sets in. The mundane is forgotten. Till of course the next tikka or burger or samosa.
The other thing that happens is self-medication. So we just pop in one pill of antacid or so, “one for the road”, and make the most out of life.
That’s quite all right. That’s exactly what 99.9%of us will do. And life shall go on. Till we cross those golden days of being a student, carefree, binge eating and dieting all at the same time. As we cross the late 20’s and step into 30’s this post-meal heaviness begins to worry us enough to consult a physician once or twice a year. As it so often happens the doctor advises an ultrasound abdomen, because the pain and bloating after meals just won’t go away. And surprise!
Prevalence, or let us say the probability of a person from the Gangetic Belt of North India of having gallstones is about 7% in those with symptoms and 3% without, with an overall average of 4%. Women more than 50 years of age, with multiple childbirths, a positive family history of gallstones and overweight have a natural predisposition to having gallstones. Diabetes and poor hygienic conditions also play a role.
Why do Gall Stones form?
Well, it is actually a lot of chemistry and biochemistry. If you are a science buff this shall be interesting. Cholesterol is the most common building block for gall stones. Now cholesterol is a naturally hydrophobic molecule (science buffs take note). It hates water but manages to remain in suspension in body fluid by the formation of micelles. Cholesterol is also the main building blocks for bile acids that get secreted from the liver and help us digest the fat in our food. Then how does it end up as stones?
Alterations in the relative or absolute proportions of cholesterol, phospholipids, and bile salts that make up the bile secretion from the liver, can lead to separation of cholesterol from solution in bile. Most frequently these changes result from excess secretion of cholesterol from the liver. As the absolute cholesterol concentration increases, the excess cholesterol phase separates. Under suitable physicochemical conditions, these can aggregate to form multilamellar liquid crystals, and eventually, cholesterol monohydrate crystals can separate from these and aggregate in the gallbladder. These crystals can progress to form cholesterol gallstones by clubbing with the mucin gel secreted from the wall of the gallbladder. Thus, the formation of cholesterol gallstones invariably occurs adjacent to the gallbladder wall.
Pure cholesterol crystals forming stones in the gallbladder are rarely seen. Mostly these are a mixed variety of stones that may brown or black or even pearly white. So, some are due to calcium salt deposition or due to bilirubin deposition along with cholesterol and calcium. Some are also due to bacterial infection within the bile system producing characteristic brown pigment stones.
What are the chances that I may have gallstones?
Community studies across the population have identified several risk factors among individuals for forming gallstones.
Age: All epidemiological studies showed that increasing age was associated with an increased prevalence of gallstones. Gallstones are 4-10 times more frequent in older than younger subjects.
Gender: In all populations of the world, regardless of overall gallstone prevalence, women during their fertile years are almost twice as likely as men to experience cholelithiasis. This preponderance persists to a lesser extent into the postmenopausal period, but the sex difference narrows with increasing age.
Parity and oral contraceptives: Increased levels of the hormone estrogen, as a result of pregnancy or hormone therapy, or the use of combined (estrogen-containing) forms of hormonal contraception, may increase cholesterol levels in bile and also decrease gallbladder movement, resulting in gallstone formation.
Genetics: Cholesterol gallstone prevalence varies widely, from extremely low (<5%) in Asian and African populations, to intermediate (10-30%) in European and Northern American populations, and to extremely high (30-70%) in populations of Native American ancestry (Pima Indians in Arizona, Mapuche Indians in Chile).
Obesity and body fat distribution: Obesity is an important risk factor for gallstone disease, more so for women than for men. It raises the risk of cholesterol gallstones by increasing the secretion of cholesterol in bile. Epidemiological studies have found that the risk of obesity being the cause of the formation of gallstones is the strongest in young women and that slimness protects against cholelithiasis.
Rapid weight loss: Rapid weight loss is associated with occurrence of sludge and gallstones in 10-25% of patients in a few weeks of initiating the slimming procedures. If a person loses weight too quickly, the liver secretes extra cholesterol; in addition, there is a rapid mobilization of cholesterol from fat tissue stores. In fasting associated with severely fat-restricted diets, gallbladder contraction is reduced, and the accompanying bile stasis in the gallbladder favors gallstone formation. Enhancing gallbladder emptying by inclusion of a small amount of dietary fat inhibits gallstone formation in patients undergoing rapid weight loss. Younger women with gallstones were shown to be more prone to skip breakfast than controls. Shorter overnight fasting is protective against gallstones in men and women.
Diet: Nutritional exposure to the western diet, i.e., increase intake of fat, refined carbohydrates and decrease in fibre content is a potent risk factor for the development of gallstones. Adequate Calcium intake in the diet protects us against gallstone formation by decreasing the cholesterol saturation in the bile. Vitamin C influences to prevent formation of gallstones in adults. Coffee consumption seems to have protective action against cholesterol stones. Coffee components enhance gallbladder motility, inhibit gallbladder fluid absorption, decrease cholesterol crystallization in bile and perhaps also increase intestinal motility.
Physical activity: Regular exercise, in addition to facilitating weight control, alone or in combination with dieting, improves several metabolic abnormalities related to both obesity and cholesterol gallstones.
Diabetes: People with diabetes generally have high levels of fatty acids called triglycerides. These fatty acids may increase the risk of gallstones. Gallbladder function is impaired in the presence of diabetic neuropathy, and regulation of hyperglycemia with insulin seems to raise the lithogenic index.
I have Gallstones! So what?
Most people who have gallstones don't know it. Their gallstones stay silent and may only be discovered incidentally, through an ultrasound or CT scan performed for other reasons. Now the question is: How shall I know that my gallstones are causing trouble?
Research has shown that about 2 to 4 out of 100 people with gallstones have noticeable symptoms within one year. About 70 out of 100 people who have already had symptoms like colic will get them again within two years. Whether someone has symptoms and what kind of symptoms they have will depend on where the gallstones have formed, how large they are, and whether they are causing any complications. If you have symptoms of gallstones, it's important to get an accurate diagnosis in order to rule out any other possible causes.
The most typical sign of gallstones is very unpleasant, cramping pain in the upper abdomen. This is called biliary colic. This pain occurs if the gallbladder is contracting to squeeze bile into the bowel, but gallstones are blocking the exit at the same time. The pain comes in waves often accompanied by nausea and vomiting, and usually gets a bit better after about an hour, eventually disappearing completely a few hours later. The pain may radiate into your right shoulder and back. Often, attacks occur after a particularly fatty meal and almost always happen at night.
Gall bladder stones can also cause other symptoms, including feeling too full, flatulence, nausea, vomiting, and regurgitation.
Between 1 percent and 3 percent of people with symptomatic gallstones develop inflammation and infection of the gallbladder (acute cholecystitis), which occurs when stones or sludge block the duct. The symptoms are similar to those of biliary colic but are more persistent and severe. They include pain in the upper right abdomen that is severe and constant and may last for days. Pain frequently increases when drawing a breath. About a third of patients have fever and chills. Nausea and vomiting may occur.
Chronic gallbladder disease involves gallstones and mild inflammation. In such cases, the gallbladder may become scarred and stiff. Symptoms of chronic gallbladder disease include complaints of gas, nausea and abdominal discomfort after meals and chronic diarrhea.
Surgery or No Surgery ?
Key points to note:
- If you feel comfortable managing mild and infrequent gallstone attacks, and if your doctor thinks that you aren't likely to have serious complications, it's okay not to have surgery.
- Most doctors recommend surgery if you have had repeated attacks. If you have had one attack of gallstone pain, you may want to wait to see whether you have more.
- Surgery is the best way to prevent gallstone attacks. The surgery is very common, so doctors have a lot of experience with it.
- Your body will work fine without a gallbladder. There may be small changes in how you digest food, but you probably won't notice them over a period of time.
There is little risk in not having surgery if you have only one mild attack. But if you have more than one painful attack, you're likely to have more in the future.
The risks of not treating gallstones may include:
- Unpredictable attacks of gallstone pain.
- Episodes of inflammation or serious infection of the gallbladder, bile ducts, or pancreas.
- Jaundice and other symptoms caused by blockage of the common bile duct. Jaundice makes your skin and the whites of your eyes yellow. It can also cause dark urine and light-coloured stools.
About 1 out of 3 people with gallstones who have a single attack of pain or other symptoms do not have symptoms again. That means that 2 out of 3 people do have another attack.
Having said all that may have been there to say, it should be pointed out that in a few circumstances early elective surgery for gallstones is advised. Thus, patients who are diagnosed with Diabetes shall be more prone to complications characterized by acute cholecystitis progressing to empyema with or without gangrene of the gallbladder. Such a clinical scenario leads to gallbladder perforation, and the resulting systemic infection is documented as life-threatening. Patients who are found to have gallstones and are due for chemotherapy or bariatric surgery (weight loss surgery) are advised elective cholecystectomy. Personnel of the Air Force, Navy and Merchant Navy are advised prophylactic surgery prior to flight/ offshore duties.
It shall be worth pointing out that having had gallstones form in the gallbladder has two main probabilities that may decide future risk events. A single gallstone that remains solo and gradually enlarges in size of more than 2cm has been well documented in the medical literature as a risk factor for the development of cancer of the gallbladder. Multiple small gallstones as they keep forming may slip down the cystic duct into the common bile duct causing severe bile duct and liver infections with jaundice. This may also result in pancreatitis which in turn may turn life-threatening.
The other reasons for advising an elective surgery for gallstones include polyps in the gallbladder as documented on ultrasound, porcelain gall bladder (that may be a malignancy), individuals with gallstones living in geographic areas with a high prevalence of gallbladder cancer.
Finally, the decision for the need for surgery your gall stones are best judged by your primary treating physician or surgeon, who has your best interest at heart.
Well, it is actually a lot of chemistry and biochemistry. If you are a science buff this shall be interesting. Cholesterol is the most common building block for gall stones.
NOTICE BOARD
CONTACT US
CONTACT US
 Book Appointment
Book Appointment

.svg)
.svg)
.svg)
.svg)








