Failed Back Surgery Syndrome (FBSS) Treatment & Diagnostics in Sadashiv Peth, Pune
Failed Back Surgery Syndrome (FBSS)
Also known as a post-laminectomy syndrome, failed back surgery syndrome (FBSS) is a condition where the patient suffers from persistent back pain following surgery of the back, generally a laminectomy.
Spinal surgery is typically performed to correct anatomical problems in the spine that cause pain. The methods used for that include decompressing pinched nerves, fixing deformed structures, and stabilizing the spine for safe movement. A laminectomy includes removal of the posterior portion of the vertebra (lamina) to create space. The spinal canal is enlarged in a laminectomy to relieve pressure on the nerves or spinal cord.
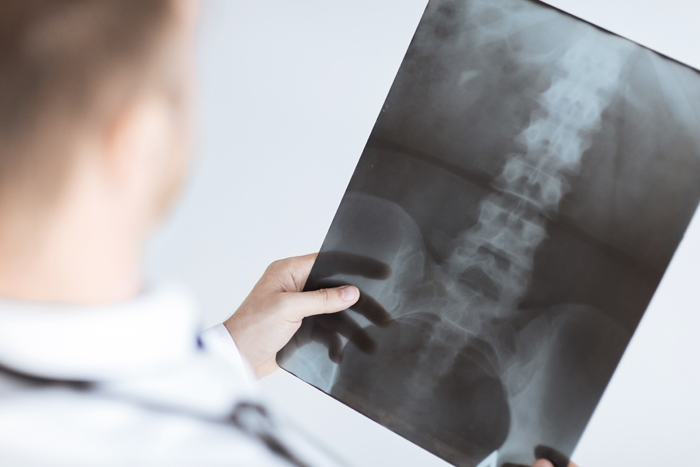
Causes
Persistent pain after spinal surgery or laminectomy can be attributed to various factors. The exact cause of failed back surgery syndrome is not known. However, these factors might cause it:
- Unnecessary surgery
- The outcome that was expected didn’t result from surgery
- Narrowing of the spinal column, known as spinal stenosis
- Sometimes, the spinal nerve root, which has been decompressed by the surgery, doesn’t recover from its prior trauma and continues to be a source of chronic nerve pain or sciatica.
- Structural changes in the spine that develop below or above the sight of spinal fusion can also cause pain.
- Scar formation around the nerve roots can also cause chronic pain.
- Postoperative spinal or pelvic ligament instability, recurrent or new disc herniation, and myofascial pain can also cause
Post-laminectomy syndrome.
Although it most commonly occurs after spinal fusion surgery, it can also be caused by:
- Incomplete removal of the lamina
- Epidural fibrosis
- Structural spinal column changes
- The progressive degeneration of the spine
- Surgical intervention at the wrong spinal level
- Recurrent disc herniation
- Infection in the epidural space or disc space
- Inflammation of the arachnoid (the membrane that surrounds the spinal cord)
Symptoms
The most obvious symptom of failed back surgery syndrome is back pain at the site of surgery accompanied by leg pain. Due to this, patients are not able to perform their daily activities and also have trouble while sleeping. Symptoms include:
- Pain similar to what one experiences before surgery
- Sharp, stabbing, pricking pain – referred to as neuropathic pain
- Sharp pain in the legs
- Dull and achy pain located in the spinal column after surgery
Diagnosis
To diagnose FBSS, your doctor will ask you about your symptoms, medical history as well as your back surgery. Additional tests might be performed to understand the symptoms and pain.
- Medical history – A review of your medical history can help your doctor to diagnose failed back surgery syndrome and any spinal disorder. You should inform your doctor about any allergies, previous and current diagnoses such as diabetes or cardiovascular disease, prescription or OTC medications that you take, including vitamin and other supplements.
- Physical exam – After this, your doctor will perform a physical exam of your spine to identify areas of tenderness, swelling, or spasms. You might also be asked to walk, bend, twist, or stand to check the range of motion, identify gait problems and test the balance, spinal alignment, and posture.
- Neurological exam – To gauge the health of your nerves and identify areas of nerve dysfunction, a neurological exam is also performed. It is also used to identify muscle weakness, radiculopathy, and abnormal sensations.
- Imaging tests – Imaging tests such as MRI, CT scan, and x-rays would be performed to confirm a diagnosis.
Treatment
Depending on each patient and the severity of pain, there can be various treatment options for Post-laminectomy syndrome, such as:
- Physical therapy and specialized exercises – Exercise and therapy that is designed to correct posture as well as strengthen the muscles supporting the back can be essential for treating FBSS.
- Anti-inflammatory medications – Non-steroidal anti-inflammatory drugs (NSAIDs) are used, sometimes along with other therapies to treat FBSS. This is the only treatment required in some cases.
- Spinal cord stimulation – In this treatment option, electrodes are placed into the epidural space of the spinal cord in the area where the pain is occurring. These electrodes will apply an electric current to interfere with pain conduction pathways.
- Facet joint injections – A local anesthetic injection combined with anti-inflammatory medication helps relieve swelling and pain in the back.
- Adhesiolysis – This is a special process wherein any fibrotic scar tissue that may have developed after surgery is removed chemically or mechanically.
- Epidural nerve block – In this process, an injection of medication is inserted into the epidural space of the spinal column for pain relief. Three to six injections would be given over six months.
- Radiofrequency neurotomy – In this procedure, the nerves are deadened with thermal energy. This procedure can provide pain relief for six to twelve months.
- Specialized inhibitors – In this process, a chemical mediator TNF-a that might be responsible for inflammatory spinal pain, is combatted.
Request an appointment at Apollo Spectra Hospitals, Swargate, Pune
Call 1860-500-2244 to book an appointment
The name is a misnomer since FBSS is not a syndrome. It is a term used to describe the condition of patients who haven’t had a successful outcome after spinal or back surgery and have experienced persistent pain.
Studies have shown that individuals who smoke are more likely to develop failed back surgery syndrome post-surgery. This is because nicotine interferes with bone metabolism and smoking can also lead to increase scar tissue build-up due to the constriction of blood vessels. Hence, to avoid failed back surgery syndrome, one should avoid smoking post back surgery.
Risk factors for FBSS include –
- Obesity
- Smoking
- Mental or emotional disorders such as anxiety or depression
- Chronic pain related to other conditions such as fibromyalgia
- Inadequate or excessive spinal decompression during surgery
- Incorrect surgery
- Recurrent original diagnosis
- Spinal infection
- Pseudoarthrosis
- Epidural fibrosis
- Adjacent segment disease
Our Doctors
DR. UTTAM ANANT SIDHAYE
MBBS, MD, FIAPM...
| Experience | : | 21 Yeras Experience |
|---|---|---|
| Speciality | : | Pain Management... |
| Super Speciality | : | Location | : | Sadashiv Peth |
Our Top Specialities
NOTICE BOARD
CONTACT US
FOR PARTNERSHIP
CONTACT US
FOR PARTNERSHIP
 Book Appointment
Book Appointment


.svg)
.svg)
.svg)
.svg)








