KERATOPLASTY Treatment & Diagnostics in Sadashiv Peth, Pune
KERATOPLASTY:
The cornea is the part of the eyes that appear white but is transparent. It has a shape like a dome. It positions itself in the outer part of the eye from which light enters from this region, enabling us to see things. Sometimes due to disease, injury, or a hereditary condition, the cornea can get affected. When such a condition occurs, you will need to go for keratoplasty.
What is keratoplasty?
Keratoplasty is popularly known as a cornea transplant. A person with almost no vision, extreme eye pain, or persistent disease in the cornea can go for keratoplasty. Here, the surgeon uses a donor's eyes and takes out the corneal tissues from it. After this, he surgically changes the corneal tissues of the patient with the donor's one.
How to prepare yourself before you undergo keratoplasty?
- Your doctor will run you through an eye examination to evaluate if complications can arise during keratoplasty.
- Your doctor will enquire about all the medicines you take. He can also ask you to stop taking some drugs before the surgery.
- Your doctor will measure the size of your eyes. This process will help him evaluate the measurement of the cornea you will need from the donors.
- If you have eye infections or other diseases, your surgeon will treat that first to ensure a smooth keratoplasty treatment.
How do surgeons perform keratoplasty?
Your surgeon will give you general or local anesthesia during the procedure.
Your surgeon will perform any one of these:
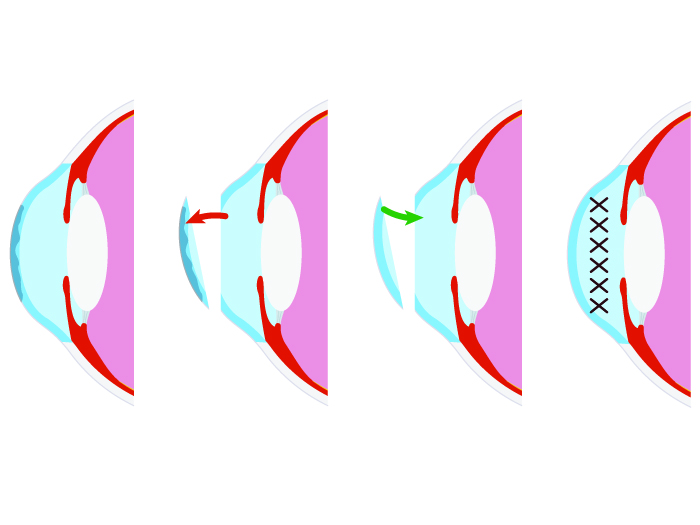
- Penetrating keratoplasty:
- This procedure is a full-thickness keratoplasty.
- The surgeon uses an instrument to cut through the thick layers of the cornea to remove all of the damaged corneal tissues.
- The cornea of the donor is then fitted in the opening.
- The surgeon will stitch the new cornea in your eyes.
- Endothelial Keratoplasty:
- The surgeon takes out the damaged tissues from the backside of the corneal surface.
- He also removes the endothelium along with the Descemet membrane (thin layer protecting the endothelium). The endothelial keratoplasty has two types: Descemet stripping endothelial keratoplasty and Descemet membrane endothelial keratoplasty. In the former, the surgeon uses the corneal tissues of the donor to change one-third of the patient's tissues. In the latter, the surgeon takes out thin and fragile layers of corneal tissues to surgically use for the patient.
- Anterior Lamellar Keratoplasty:
- The surgeon leaves the endothelium but takes out the damaged tissues from the front part of the eyes (stroma and epithelium).
- The surgeon can perform any one of the Anterior Lamellar Keratoplasty.
- Superficial Anterior Lamellar Keratoplasty
- Deep Anterior Lamellar Keratoplasty.
- In the former, the surgeon changes only the front and upper layers of the cornea and does not touch the stroma. In the latter, the surgeon uses the donor's healthy tissues to replace the damaged corneal tissues till the stroma.
When to see your doctor?
When your body rejects a cornea after keratoplasty, you will face several issues, and you will need to see a doctor. These symptoms include:
- Redness.
- Loss of vision.
- Pain and swelling in the eyes.
- Sensitivity to light.
Request an appointment at Apollo Spectra Hospitals, Pune
Call 1860-500-2244 to book an appointment
How does recovery look after keratoplasty?
- He will also prescribe follow-up medication to ensure you don't feel pain or swelling in the eyes.
- You will need to ensure that you do not injure your eyes. Don't rub and press them and take time to return to your daily chores.
- You will need to wear glasses or eye shields to protect your eyes.
- You will need to visit your doctor regularly to check for complications.
Conclusion:
Those who undergo keratoplasty get their vision back fully or partially. You will need to visit your doctor often to ensure no complication arises after keratoplasty. You will be at risk for several years, so ensure you keep going to your doctor.
- If your cornea is swelling.
- If you have keratoconus or a bulging cornea.
- If you experience a tear in the cornea due to an injury.
- When the opthalmologist detects you with an eye ulcer, but medical treatment fails.
- If you have a hereditary condition called Fuch's dystrophy.
Surgeons practice corneal transplant or keratoplasty widely. Often, the donors are dead people with healthy cornea. The surgeon does not use the cornea of people who died from diseases or other ailments. Tissue matching is not a requirement, and hence, donor corneas are available most of the time.
Usually, the effect of keratoplasty is long, and it will last you throughout your life. At times, due to rejection from the patient's body, you will need to replace them again. This condition can occur during the surgery, after it, or even ten years down the line. In rare cases, the corneal tissues of the donor might fail to work. This condition occurs if the donor was aged and not healthy.
Our Doctors
DR. VANDANA KULKARNI
MBBS, MS, DOMS...
| Experience | : | 39 Yeras Experience |
|---|---|---|
| Speciality | : | Ophthalmology... |
| Super Speciality | : | Location | : | Sadashiv Peth |
Our Top Specialities
NOTICE BOARD
CONTACT US
CONTACT US
 Book Appointment
Book Appointment


.svg)
.svg)
.svg)
.svg)








