Keratoplasty Treatment & Diagnostics in Tardeo, Mumbai
Keratoplasty
A damaged cornea can cause a lot of pain and even vision loss. The damage can include thinning, bulging, dystrophy, scarring, swelling or clouding of the cornea. Such damage cannot be healed. In such cases, surgical procedures like keratoplasty can help you regain vision.
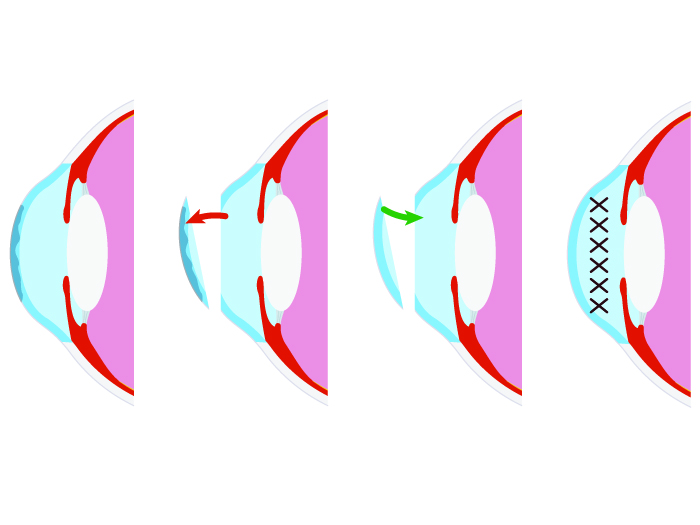
What do we need to know about keratoplasty?
The dome-shaped transparent top surface of your eyes is the cornea. The light enters your eyes through the cornea and your ability to see clearly is very much dependent on its health. If your cornea is damaged or diseased, it can cause a lot of pain or even result in vision loss.
The surgical procedure to replace part or full thickness of your cornea with corneal tissues obtained from a donor is called keratoplasty or cornea transplant surgery.
Keratoplasty can restore vision.
To seek treatment, you can visit any ophthalmology hospital in Mumbai. Or search online for an ophthalmology doctor near me.
What are the types of keratoplasty?
Depending on the condition of your cornea, a keratoplasty specialist will choose one of the following types of keratoplasty:
- Penetrating keratoplasty – This involves the transplant of the entire thickness of the abnormal cornea.
- Descemet stripping endothelial keratoplasty – Back layer of the cornea is replaced.
- Descemet membrane endothelial keratoplasty - Very thin membrane of the back layer of the cornea is transplanted.
- Superficial anterior lamellar keratoplasty – Replaces thin front layers of the cornea.
- Deep anterior lamellar keratoplasty – Transplant of front layers in which the damage has spread a bit deeper.
What are the symptoms that indicate that you need keratoplasty? Why is this procedure needed?
A cornea transplant is suggested by an ophthalmologist or a keratoplasty specialist to those who have lost partial or complete vision due to damaged cornea. This condition can be a birth defect or may arise due to some injury or infection.
Those who have one or more of the following conditions may need keratoplasty:
- Scarred cornea due to injury or infection
- An outward bulge in the cornea
- Swollen cornea
- Thin or torn cornea
- Heredity condition like Fuchs’ dystrophy
- Complications in the cornea due to past eye surgeries
- Clouding of cornea
- Corneal ulcers
When do you need to see a doctor for keratoplasty?
Keratoplasty is a relatively low-risk procedure. If you are suffering from any of the conditions mentioned above, you would need a cornea transplant. Corneal conditions can be found out during your regular eye check-ups. If he/she finds some abnormalities, your ophthalmologist may suggest that you visit a keratoplasty hospital for further diagnosis and treatment.
You can request an appointment at Apollo Spectra Hospitals, Tardeo, Mumbai.
Call 1860 500 2244 to book an appointment.
What are the complications?
Keratoplasty is considered a safe surgical procedure. But there can be some complications. For instance, your immune system may consider the donor cornea as a threat and attack the tissue.
Most of the complications of keratoplasty can be prevented or managed effectively by following your doctor’s recommendations, follow-up check-ups and proper care. Here are a few common complications:
- Retinal detachment
- Swelling of the retina
- Eye infection
- Bleeding
- Increase in intraocular pressure
- Clouding of the natural lens
- Issues with stitches
- Rejection of donor cornea
How is keratoplasty performed?
For the keratoplasty procedure, the corneas used to replace the damaged corneal tissues come from human donors. Corneas are taken from donors whose medical history is known and who haven’t had any eye disease or surgery antemortem.
Depending on the depth of the damage in the cornea, your surgeon decides the thickness of the cornea to be replaced and chooses the procedure accordingly. Keratoplasty is usually an outpatient procedure performed under local anesthesia. Surgery is done on one eye at a time, so you may go home the same day. That depends on your condition.
Whether it is penetrating keratoplasty involving full-thickness cornea transplant or partial cornea transplant like endothelial or anterior lamellar keratoplasty, the general process more or less remains similar. The surgeon cuts and removes abnormal or affected layers of the cornea and replaces them with healthy donor tissues. The replaced cornea is kept in place using sutures.
Conclusion
Keratoplasty can be a blessing for those who have suffered significant vision loss due to damaged or diseased cornea. It may take up to a year to fully adapt and function optimally, and the results may vary depending on many factors, but it will surely help restore vision at least partially. With proper care and guidance from doctors, the improved vision after keratoplasty can last a lifetime.
Largely the rejection occurs due to neglecting the suggested precautions, ignoring follow-up visits or failing to take the prescribed medication.
No. Keratoplasty is a procedure to replace the cornea which itself is clear, so it won’t alter the eye color.
Yes. With proper medication and care, there is a significant chance of reversing corneal rejection.
Our Doctors
DR. NEETA SHARMA
MBBS, DO (Ophthal), ...
| Experience | : | 31 Yeras Experience |
|---|---|---|
| Speciality | : | Ophthalmology... |
| Super Speciality | : | Location | : | Chembur |
DR. PALLAVI BIPTE
MBBS, MS (Ophthalmol...
| Experience | : | 21 Yeras Experience |
|---|---|---|
| Speciality | : | Ophthalmology... |
| Super Speciality | : | Location | : | Chembur |
DR. NUSRAT BUKHARI
MBBS, DOMS, Fellowsh...
| Experience | : | 12 Yeras Experience |
|---|---|---|
| Speciality | : | Ophthalmology... |
| Super Speciality | : | Location | : | Tardeo |
Our Top Specialities
NOTICE BOARD
CONTACT US
FOR PARTNERSHIP
CONTACT US
FOR PARTNERSHIP
 Book Appointment
Book Appointment




.svg)
.svg)
.svg)
.svg)








